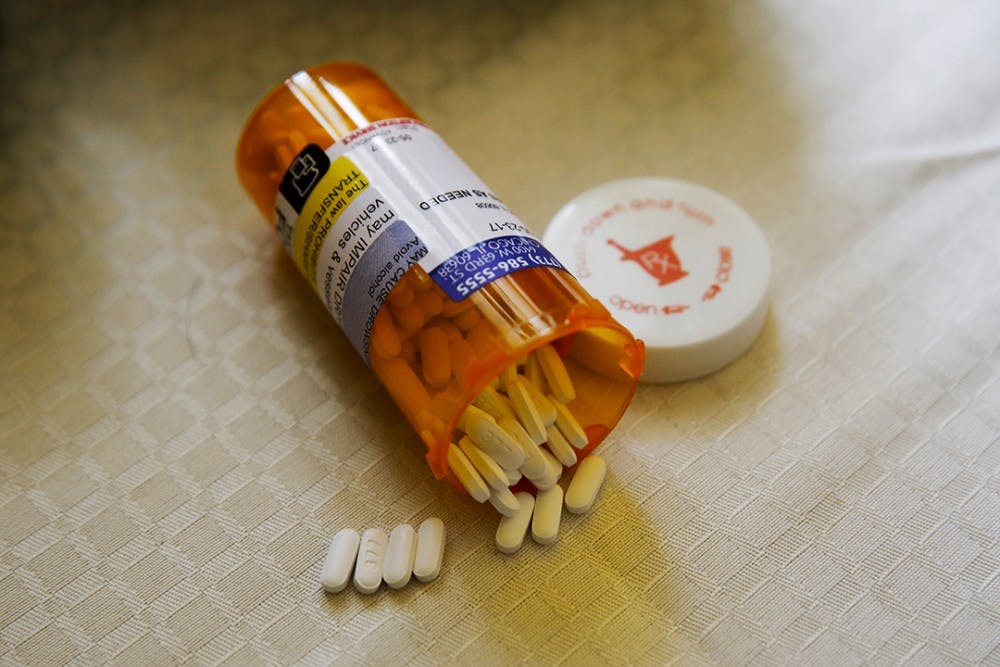
A USC assistant professor and her students are helping to shape the country's response to a nationwide addiction crisis with a new study published in the Health Affairs Journal after studying Medicaid and its provisions for addiction treatment.
Christina Andrews, an assistant professor in the College of Social Work, led a team of researchers to highlight expanded Medicaid addiction treatment under the Affordable Care Act. Melissa Westlake, a Ph.D. student in the College of Social Work, aided Andrews in the research.
Medicaid is the largest funder of mental health services and is increasing its role in addiction treatment.
“However, addiction treatment has often been subject to limits on benefits and use that are inconsistent with clinical recommendations and more restrictive than those placed on other medical services,” the study reads.
The Affordable Care Act established a set of essential health benefits that states are required to offer and extend the reach of the Paul Wellstone and Pete Domenici Mental Health Parity and the Addiction Equity Act of 2008, which expanded addiction treatment for patients. The 2008 law is responsible for reducing the limitations on addiction treatment benefits as well.
The study "assessed changes in addiction treatment benefits and utilization controls on their use in standard Medicaid and alternative benefit plans."
The researchers used data from the National Drug Abuse Treatment System Survey which conducts nationally representative surveys periodically and has done so since 1984.
The team studied data from 2014 to 2017 and conducted an internet-based survey of Medicaid programs in all 50 states and the District of Columbia to determine if their addiction treatment benefits were indeed expanded. 47 Medicaid programs responded to their survey, and the study found that expansion did happen.
“The proportion of state plans that provided benefits for residential treatment and opioid use disorder medications increased from 2014 to 2017,” the study reads.
Medicine coverage was the area that had the largest increase. Treatments like methadone, which increased from 33 to 40 state plans, and oral naltrexone which increased from 37 to 45 states, saw major expansion.
“This study indicates that benefits for substance use disorder treatment have improved substantially since key provisions of the Affordable Care Act went into effect in 2014," Andrews said.
She also pointed to the current opioid epidemic which gained traction and focus in the last presidential election.
"Expanding access to substance use disorder is critically important as the nation struggles to respond to an escalating opioid epidemic,” Andrews said.
Andrews's study points to Medicaid as the impetus in tackling opioid use disorder at a higher rate.
“The biggest impacts that we’re seeing and the biggest expansion in coverage and greater access to coverage is really in these states where Medicaid has been expanded,” Westlake said.
Andrews said the study has the potential to help experts understand how improvements in care affect people's access to care.
“It will be important to understand how improvements in benefits in substance use disorder treatment influence the ability of Americans covered by Medicaid to access care," she said. "For example, do more people access care? Do they stay in treatment longer?”
Sarah Gehlert, dean of the College of Social Work, said studies like this help translate teaching and research into action.
“Publishing results in high-profile journals like Health Affairs helps achieve this end by making legislators and policy makers aware of research findings that can guide their work,” Gehlert said. She said she has no doubt that Andrews’ work will have an impact on addiction treatment in the U.S.
Although this study shows improved coverage for addiction treatment, some limitations remain for those with severe addiction who require crisis stabilization and an attentive recovery environment, the study claims.
You can read the full study here.